SAN Resources

NRHI Support and Alignment Network (NRHI SAN) Resources
Included are selected materials developed by expert NRHI member faculty and based on the priority needs of the Transforming Clinical Practice Initiative Community
Bundles

Sustaining
Quality Improvement Work
The bundle includes easily accessible learning modules with short videos and key takeaways around topics related to sustaining and ongoing efforts on QI initiatives and programming.
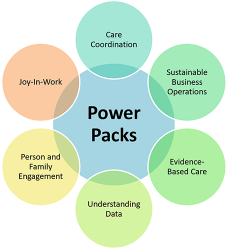
Transforming Clinical Practice Initiative (TCPi) Power Packs
Each Power Pack solves a specific challenge that a practice might face as it begins the process of clinical practice transformation. They demonstrate specific pathways to resolve healthcare delivery challenges.

Navigating the Transition to Alternative Payment Models (APMs)
Primary and specialty care providers face many challenges as they navigate the complex landscape to transition their practice from a model focused on volume, to value.
~~~
Resources from the NRHI SAN Online Community
Advancing Care Management
- ACM Module 1: Care Management Through Registries – Recording
- ACM Module 1 Slide Deck
- ACM Module 2: Power Up for Managing a Population – Recording
- ACM Module 2: Slide Deck
- Advancing Care Management – Q & A
- Advancing Care Management Resource List

Behavioral Health Integration Learning Program
- NRHI SAN Behavioral Health Integration Module Resource List
- NRHI SAN Behavioral Health Integration Q & A document reflects questions asked during Behavioral Health Integration (BHI) learning Modules: Module 1: Addressing Behavioral Health Issues in Primary Care, Module 2: Building Internal Capability, Module 3: Care Processes and Connections, and Module 4: Measuring and Improving Care for Depression.
~~~
- Milliman American Psychiatric Association Report: Economic Impact of Integrated Medical-Behavioral Healthcare- Implications for Psychiatry
- Mortality in Mental Disorders and Global Disease Burden Implications: A Systematic Review and Meta-analysis
- SAMHSA-HRSA Quickstart Guide to Behavioral Health Integration: An encyclopedic journey to Behavioral Health Integration with links to every type of resource you can imagine.
- Quality Measures Useful in Evaluating Behavioral Health Care for QI and P4P: https://search.ahrq.gov/search?q=depression
- Policy Brief 21: The Synthesis Project: New Insights From Research Results: Mental Disorders and Medical Co-morbidity. Robert Wood Johnson Foundation, February 2011
- Organized evidence-based care in Behavioral Health: A highly practical and field-tested approach from leaders in the field
- Mental Health and Chronic Disease, CDC Issue Brief NO.2, October 2012
- Issue Brief: Fixing Behavioral Health Care in America. The Kennedy Forum, 2015
- Evolving Models of Behavioral Health Integration: Evidence Update 2010-2015
- Collaborative Care Management: The evidence-based approach to depression in primary care
- CMS Video on Interviewing Vulnerable Elders (VIVE):
Depression screening tutorial produced by CMS (Published on Sep 2, 2010)
The systematic inclusion of resident voice through specific direct interviews represents an enormous advance in the new Minimum Data Set 3.0 (MDS 3.0). The Video on Interviewing Vulnerable Elders (VIVE) demonstrates best practice approaches for implementing the new MDS interviews for cognition, mood, preferences and pain. Specific video sections address the reason interviews have been added, techniques to improve communication with older, frail populations, and demonstration of each interview being conducted. Using real life nurses interacting in scenarios based on actual situations, VIVE helps to build understanding and ease implementation of MDS 3.0 for nursing home staff members. The goal of VIVE, funded by the Picker Institute and developed by the UCLA/Jewish Home Borun Center, is to help staff members build the confidence and skills they need to interview their residents both for MDS 3.0 and for other clinical evaluations. Watch video.
- Behavioral Health Integration and PCMH: Connects the PCMH work already underway to behavioral health integration efforts
- CDC Step-by-step guide for Primary Care Practices: Alcohol Use Screening, Brief Intervention, Referral and Treatment:
- Coding for chronic care and behavioral health integration:
- RE: Two follow-up questions for Dr Block
- Follow-up resources from BHI Module 2:
- APA’s SAN will worked closely with the AIMS Center at the University of Washington to train a network of 3,500 psychiatrists in the Collaborative Care Model and will provide those psychiatrists with the clinical and leadership skills needed to support primary care practices that are implementing integrated behavioral health programs. https://www.nrhi.org/uploads/apa-san-slide-for-nrhi.pdf
- Behavioral Health Integration Module 1: Slide deck
- Behavioral Health Integration Module 1: Video Recording (March 24, 2016)
- Behavioral Health Integration Module 2: Slide deck
- Behavioral Health Integration Module 2: Video Recording
- Behavioral Health Integration Module 3: Slide deck
- Behavioral Health Integration Module 3: Video Recording
- Behavioral Health Integration Module 4: Slide deck Program launched 12/01/2016
- Behavioral Health Integration Module 3: Video Recording (aired on 12/01/2016)
Improving Person and Family Engagement
- Access the slide deck from this module launched on 06.22.2017
- Access the video recording of the event launch on 06.22.2017
On June 22nd, 2017 MHQP hosted a conversation in which we described our patient experience surveying program and how to use the results to improve quality. We were joined by leaders at two provider organizations that have real world experience in working with their staffs to use PES results to provide more patient-centered care. Each has seen its scores and its patients’ experience improve dramatically over time.
Suzanne Countie from Lowell General PHO talked about how important it is to make a connection with the patient, and that it all starts with empathy. Check out this Cleveland Clinic Video: Empathy: The Human Connection to Patient Care. Dr. Hartmann talked about as pecific program developed for asthma that resulted in his practice having the lowest emergency room visits for children with asthma among all the practices in the Pediatric Physicians’ Organization at Children’s (PPOC).
Check out the recording from our live event here: NRHI SAN: How to Help Clinicians Take Action with their PES Results. Additional resources, including the slide deck from the event, and a Q and A document coming soon, can be in the Resources section in this group.
Survey templates available from AHRQ CAHPS that you might want to use include:
- CAHPS Patient Narrative Elicitation Protocol(beta version): A structured series of five open-ended questions to gather narrative comments from patients.
- CAHPS Patient-Centered Medical Home (PCMH) Item Set
- CAHPS Health Literacy Item Set
- CAHPS Health Information Technology Item Set
Key takeaways from the presentation included:
- Compare your PES results to others, assess correlation of each domain with key global ratings and watch trends in results over time.
- Meet with your clinicians and other staff to interpret the practice’s Patient Experience Survey results
- Hold patient focus groups and/or meet with patients engaged in your leadership to get a more complete picture of areas where improvement is needed
- Select a focus for improvement based on all these facts and determine the interventions to be tested
- Understand how each staff member contributes to the patients’ experience and include the whole team in improvement efforts
- Implement the improvement and determine how to measure the impact of improvement efforts, make changes as needed and measure results both short term and on an annual basis
- Motivational Interviewing and Shared-Decision Making Handouts for practices
- Module 2 Slide Deck: Opportunities to Improve Care Outcomes (launched on 07.27.2017)
- Module 2 Video Recording: Opportunities to Improve Care Outcomes (launched on 07.27.2017)
- Access the slide deck from this module launched on 09.07.2017
- Access the video recording (09.07.2017)
- Advance Care Planning and End of Live Care Module 4: Slide Deck (09.13.2017)
- Advance Care Planning and End of Live Care Module 4: Video Recording (09.13.2017)
- Access all of the NRHI SAN PFE recordings, slide decks, and other resources shared throughout our program series, all in one place!:
- Compilation of all the questions and answers discussed during our live PFE events.

Reducing Unnecessary Utilization Learning Program
- Access videorecording of Module 1: Creating Clinician and Consumer Engagement to Implement Choosing Wisely in Practice
- Discussion from Module 1: Creating Clinician and Consumer Engagement to Implement Choosing Wisely in Practice.
- Access videorecording for Module 2: Creating a Transition Care Model to Improve Care Coordination
- Access Q and A discussion for Module 2
- Slide Deck: NRHI SAN Reducing Unnecessary utilization Module 3: Empowering Clinicians to Reduce Unnecessary Care: Understanding Practice Pattern Variation
- Recording for Module 3
- Q and A document compiled from discussion during live event on November 15, 2016.
- Access Module 4 Strategies for clinics to address imaging for low back pain and cost of care Q & A file
- Access Module 4 Slide Deck
- Access Module 4 Video Recording
- Access Module 5 Improving Access to Specialty Care to Reduce Unnecessary ED Visits Q & A file
- Access Module 5 Slide Deck
- Access Module 5 Video Recording
- Access Module 6 Advance Care Planning & POLST: A Strategy to Address Re-Admissions Q & A file
- Access Module 6 Slide Deck
- Access Module 6 Video Recording
- Access Module 7 Understanding and Facilitating the Role of Specialists and Sub Specialists in Preventing Unnecessary Hospital Care Slide Deck
- Care Transitions Intervention (Coleman)
- Project Boost Implementation Toolkit:
The BOOSTing (Better Outcomes by Optimizing Safe Transitions) Care Transitions implementation toolkit provides a wealth of materials to help you optimize the discharge process at your institution.
The tools and approach are based on principles of quality improvement (QI), evidence-based medicine, as well as personal and institutional experiences.
- Re-Engineered Discharge (RED) Toolkit:
- Project RED is an AHRQ-funded intervention which seeks to reduce hospital readmissions through the redesign of hospital discharge processes. A hallmark of the initiative is its use of a nurse “discharge advocate” who follows eleven discrete, mutually-reinforcing action steps: (1) educate the patient about his/her diagnoses throughout the hospital stay; (2) make appointments for clinician follow-up and post-discharge testing; (3) discuss with the patient any tests or studies that have been completed in the hospital and discuss who will be responsible for following up the results; (4) Organize post-discharge services; (5) confirm the medication plan; (6) reconcile the discharge plan with national guidelines and critical pathways; (7) review the appropriate steps for what to do if a problem arises; (8) expedited transmission of the Discharge Resume (summary) to the PCP/physicians accepting responsibility for the patient’s care after discharge; (9) assess the patients’ degree of understanding by asking them to explain the details of the plan in their own words; (10) give the patient a written discharge plan at the time of discharge; and (11) telephone re-enforcement of the discharge plan and problem solving 2 to 3 days after discharge.
- Caregivers of Older Adults: A Focused Look at Those Caring for Someone Age 50+
- Why Avoid The Hospital
- 30 Day Readmission Rates to US Hospitals infographic
Watch NRHI’s vlog on how Choosing Wisely can help patients and doctors avoid unnecessary and costly care. This is one way to advance healthcare affordability.

