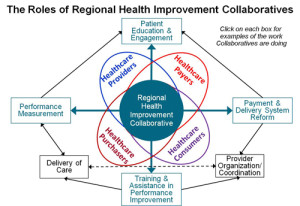
 Although measurement, reporting and changes in payment systems are necessary to support higher-value healthcare delivery, improvements in quality, efficiency, and patient satisfaction are actually achieved through the actions of front-line healthcare workers. Regional Health Improvement Collaboratives operate programs designed to improve the way that physicians, nurses, hospital administrators, and other healthcare professionals deliver care, ranging from identifying and disseminating best practices in care delivery, to providing affordable training, coaching, and technical assistance to practitioners on ways to analyze problems in care delivery and ways to design and successfully implement solutions, to helping healthcare providers reorganize and modernize their operations to support better-quality, more-affordable care.
Although measurement, reporting and changes in payment systems are necessary to support higher-value healthcare delivery, improvements in quality, efficiency, and patient satisfaction are actually achieved through the actions of front-line healthcare workers. Regional Health Improvement Collaboratives operate programs designed to improve the way that physicians, nurses, hospital administrators, and other healthcare professionals deliver care, ranging from identifying and disseminating best practices in care delivery, to providing affordable training, coaching, and technical assistance to practitioners on ways to analyze problems in care delivery and ways to design and successfully implement solutions, to helping healthcare providers reorganize and modernize their operations to support better-quality, more-affordable care.
The Center for Medicare and Medicaid Services (CMS) Innovation Center launched a nationwide public-private collaboration called the Hospital Engagement Networks (HEN) to identify and create innovative solutions designed to reduce patient harm and improve care coordination. CMS awarded 26 organizations a two-year contract to help identify the key improvements and spread initiatives across their defined population. The Iowa Healthcare Collaborative was awarded the sole Iowa-based contract to serve Iowa hospitals in this campaign. The 127 hospitals participating in the Iowa-based Hospital Engagement Network (HEN) prevented potential harm to more than 4,300 patients in 2013 and reduced health care costs by more than $51 million, according to data released by the Iowa Healthcare Collaborative (IHC), which administers the network. Read more.
See How our Collaboratives are Making a Difference
New Jersey Health Care Quality Institute‘s work is improving health in communities across New Jersey.
PRHI’s Perfecting Patient Care
The Pittsburgh Regional Health Initiative (PRHI) pioneered the adaptation of “lean” manufacturing from the Toyota Production System so that they could be successfully used to improve quality and reduce costs in healthcare. PRHI’s Perfecting Patient Care ℠(PPC) system has been used by hospitals, physicians, nursing homes, and other providers all over the country to achieve dramatic reductions in hospital-acquired infections, preventable hospital readmissions, pre-term deliveries of babies, and many other areas that benefit patients and reduce healthcare costs. PRHI’s Tomorrow’s Healthcare ℠ program brings Perfecting Patient Care tools to a web-based platform.
ICSI Guidelines
The Institute for Clinical Systems Improvement has developed and maintains an extensive array of guidelines for healthcare services based on the best evidence available, and then it works to help healthcare providers implement the guidelines and make other improvements in their own organizations.
Many Regional Health Improvement Collaboratives, for example Better Health Greater Cleveland, have programs designed to help providers, either individually or in groups, to better organize and deliver healthcare in order to improve quality and efficiency. Several Collaboratives, including Comagine Health in Nevada and Utah, the Louisiana Health Care Quality Forum, the Pittsburgh Regional Health Initiative, and Qualidigm, are helping physician practices become patient-centered medical homes, implement electronic health records, and more effectively coordinate care with other providers. The Iowa Healthcare Collaborative is transforming primary care in Iowa through its Medical Home Learning Community and Medical Home System Advisory Council.
Achieving Oregon’s Vision for the Triple AIM
The Patient-Centered Primary Care Institute, a public-private partnership between the Oregon Health Care Quality Corporation and the Oregon Health Authority, helps providers and practices achieve improvements in quality, access, coordination, patient experience and clinical outcomes – and thereby fulfill Oregon’s vision for the Triple Aim outcomes. Providers, clinic staff, technical experts, patient advisers, quality improvement professionals, policymakers and academic centers – all collaborate to advance and share knowledge and resources. Visit www.pcpci.org to learn more about the Institute and find valuable practice transformation resources, including a series of webinar trainings.
Status Report on Efforts to Improve Quality in Primary Care Practices through Common Table Health Alliance’s Project Better Care in Memphis and Shelby County Tennessee
The Common Table Health Alliance (previously Healthy Memphis Common Table) released a report on primary care in Memphis and Shelby County, titled “Status Report on Efforts to Improve Quality in Primary Care Practices through HMCT’s Project Better Care in Memphis and Shelby County, Tennessee,” from its Take Charge for Better Health® Series. The report highlights how quality improvement and the effective delivery of primary care can prevent emergency department (ED) visits for patients with type 2 diabetes. Download Report
Briefing Highlights on Efforts to Improve Quality in Primary Care Practices through Common Table Health Alliance’s Project Better Care in Memphis and Shelby County Tennessee
This briefing highlights the findings of the Alliance’s report on primary care in Memphis and Shelby County entitled, “Status Report on Efforts to Improve Quality in Primary Care Practices through HMCT’s Project Better Care in Memphis and Shelby County, Tennessee,” from its Take Charge for Better Health® Series. Download
Greater Detroit Area Health Council Partners for “See You in 7”
GDAHC partnered with the Michigan Chapter of the American College of Cardiology (ACC) and MPRO, Michigan’s Quality Improvement Organization, to launch the southeast Michigan “See You in 7” hospital collaborative. The purpose of the Collaborative was to improve the early follow-up process for heart failure patients. The goal of the Collaborative was to reduce readmissions. The Collaborative focused on process measures from the ACC’s toolkit to increase the number of follow-up appointments within seven days of discharge. MPRO provided data for the Collaborative, which showed that the ten hospitals participating in the Collaborative were able to reduce readmissions by 9.5% compared to 4.9% for other hospitals in the state. Details of the Collaborative are available at www.gdahc.org.
ED Use
GDAHC’s initiative focuses on reducing use of Emergency Departments for conditions that are better treated by a Primary Care Physician (PCP). Strategies include expansion of a GDAHC pilot that successfully showed there are simple actions PCPs can take, such as revising their after-hours telephone script, ensuring a written triage policy for urgent visits that all staff follow and ensuring patients are aware of ways to access PCP advice after-hours. In GDAHC’s pilot, PCP practices reduced their patients’ use of EDs for PCP treatable conditions from a high of 49.2 visits/1000 to just 7.3 visits/1000 at the end of the four-month project. In addition to PCP actions, GDAHC has a campaign to educate consumers about appropriate settings of care; GDAHC created a Stoplight poster, brochure and presentation that can be used to educate consumers. GDAHC printed 5,000 Stoplight posters of various sizes and is in the process of distributing them throughout the region to be displayed in physician practices, employee lunchrooms and other settings throughout the community so consumers get a consistent and repeated message. More information and details about the PCP pilot are available at www.gdahc.org.


