Read NRHI’s paper from its Payment Reform Series: Moving from Quality to Value: Measuring and Controlling the Cost of Health Care.
Consumers want answers to basic questions:
- How can we spend less for better healthcare?
- Are we actually getting the services that we pay for?
- What are the barriers to better healthcare?
Although performance measurement and reporting efforts have made a positive impact on quality, only so much can be done when healthcare payment systems penalize improvement and when providers’ practices impede coordination. Significant changes in the way healthcare is paid for, the way providers are organized, and the way consumer benefits are structured will be needed to achieve greater value in healthcare. To be successful, these changes must be made in a coordinated way.
In Minnesota, the “total cost of care” report, released December 18, 2014, “was billed as a major advance in the consumer health care movement — and one that would soon be mimicked by other states and federal agencies seeking to place more cost and quality data in consumers’ hands.” Read news article and read additional coverage this report is getting.
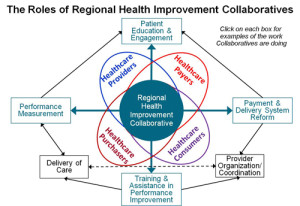
Collaboratives as Catalysts for Payment and Delivery Reform Regional Health Improvement Collaboratives can serve as catalysts for payment and delivery system reforms, as neutral planning and problem-solving forums where win-win multi-payer, multi-provider payment and delivery reforms can be designed, and as sources of both leadership and technical assistance in implementing needed reforms.
Pay-for-Performance and Performance-Based Contracting Using Collaborative-Generated Performance Measures In a number of cases, the performance measures reported by Regional Health Improvement Collaboratives are being used by employers and health plans in the community to reward providers that deliver higher-quality care and to encourage patients to use higher-quality providers. Using a common set of measures developed by the Regional Health Improvement Collaborative reduces the administrative burden for both plans and providers and encourages accelerated improvement.
See What Our Members Are Doing to Make a Difference Common Ground Health convenes the Community Technology Assessment Advisory Board, or CTAAB, that provides an independent, evidence-based appraisal of community need for new or expanded medical services, technology and major capital expenditures. Download PDF.
The Pivotal Role of Collaboratives in Designing and Implementing Fundamental Payment Reforms Regional Health Improvement Collaboratives were among the first healthcare leaders in the country to recognize that more fundamental payment reforms were needed than Pay-for-Performance systems. In 2007 and 2008, the Network for Regional Healthcare Improvement convened national Payment Reform Summits that brought together national thought leaders and regional stakeholders and made detailed recommendations on the types of reforms needed to payment systems and what was needed to successfully implement these payment reforms in regions across the country.
Building on NRHI’s national summits, a number of Regional Health Improvement Collaboratives have held regional Payment Reform Summits to build consensus in their communities on the types of payment reforms which should be implemented by all payers, so that physicians and other healthcare providers are not forced to deal with multiple, disparate new payment structures. For example:
- HealthInsight (now Comagine Health) and its Nevada Partnership for Value-Driven Healthcare held a statewide Payment Reform Summit in Las Vegas on April 22, 2010. At the Summit, 140 attendees,including healthcare provider and health plan executives, outpatient practice managers, employers and members of purchasing coalitions, consumer groups, and other interested stakeholders, developed recommendations for payment reforms to support medical homes for chronic disease patients and more efficient, successful care of major acute episodes.
A number of Regional Health Improvement Collaboratives are working with stakeholders to implement fundamental payment reforms in their communities on a multi-payer basis. For example:
- The Institute for Clinical Systems Improvement reached agreement among all of the major health plans in Minnesota on several major changes in payments to support higher-value care. The DIAMOND Initiative includes changes in payments to both primary care practices and specialists to support better care for patients with depression, and has resulted in significant improvements in remission rates. The Diagnostic Imaging Project has helped physician practices reduce overutilization of high-tech diagnostic imaging, saving tens of millions of dollars.
- The Integrated Healthcare Association has led the development of a program in California to pay hospitals and physicians for certain surgeries on a bundled episode-of-care basis.
- Qualidigm has served as the lead for Maine’s Multipayer Advanced Primary Care Program as well as the Maine Medicaid Health Homes Initiative. In the Advanced Primary Care pilot, Maine Quality Counts worked with Maine Health Management Coalition to bring all payers to the table to reach consensus on enhanced payments for medical home functions. Although each contract was negotiated directly between the parties, general agreement across payers and providers facilitated by the neutral Regional Health Improvement Collaborative on needed revenue and expected outcomes enabled the all-payer approach.
Ensuring Costs Are Not Reduced at the Expense of Quality As more communities begin efforts to develop and implement payment changes, the need for the performance measurement capabilities of Regional Health Improvement Collaboratives will grow. For example, in order to refine outcome targets and strategies for reaching them, healthcare providers need information about the current costs and outcomes associated with their patients. The data that many Collaboratives are already collecting and reporting serve as a trusted source of information that both providers and payers can use to design and implement new payment models. For example:
- The Louisiana Health Care Quality Forum’s Quality MAP (Measurement Analysis Portal) allows users to do their own analyses of healthcare claims data for Louisiana as well as to get pre-defined standard reports.
- The Pittsburgh Regional Health Initiative‘s Readmission Briefs provide guidance on the causes of hospital re-admissions for all types of patients that can help guide healthcare providers seeking to reduce them.
- Watch video on how CIVHC has been actively working with key stakeholders to expand the prevalence of new payment models.
- See how the Wisconsin Health Organization has created one of the most comprehensive sources of health claims information in the U.S. and how it is improving health care transparency.
Resolving Implementation Problems in Payment and Delivery System Reform No matter how much thought is put into designing new payment systems and delivery system reforms, implementation challenges will inevitably arise. A Regional Health Improvement Collaborative that is supported by all stakeholders and perceived as neutral can provide a critical mediation mechanism for resolving problems quickly and effectively. For example:
- Oregon Health Care Quality Corporation brings stakeholders together to produce transparent information about the quality, utilization and cost of healthcare in Oregon.